O Leukoplakia
O Hairy leukoplakia
O Lichen planus
O Lichenoid reactions
O Linea alba
O Nicotinic stomatitis
O Uremic stomatitis
O Cinnamon contact stomatitis
O Chemical burn
O Candidiasis
O Chronic biting
O Geographic tongue
O Hairy tongue
O Furred tongue
O Materia alba of the gingiva
O Fordyce’s granules
O Leukoedema
O White sponge nevus
O Dyskeratosis congenita
O Pachyonychia congenita
O Focal palmoplantar and oral mucosa hyperkeratosis syndrome
O Papilloma
O Verrucous carcinoma
O Squamous-cell carcinoma
O Skin and mucosal grafts
O Epithelial peeling
 |
| White Lesions |
Leukoplakia
Definition Leukoplakia is a clinical term, and the lesion is defined as a white patch or plaque, firmly attached to the oral mucosa, that cannot be classified as any other disease entity. It is a precancerous lesion.
Etiology The exact etiology remains unknown. Tobacco, alcohol, chronic local friction, and Candida albicans are important predisposing factors. Human papilloma virus (HPV) may also be involved in the pathogenesis of oral leukoplakia.
Clinical features Three clinical varieties (Figs. 1 and 2) are recognized: homogeneous (common), speckled (less common), and verrucous (rare). Speckled and verrucous leukoplakia have a greater risk for malignant transformation than the homogeneous form. The average percentage of malignant transformation for leukoplakia varies between 4% and 6%. The buccal mucosa, tongue, floor of the mouth, gingiva, and lower lip are the most commonly affected sites.
Laboratory tests Histopathological examination.
Differential diagnosis Lichen planus, cinnamon contact stomatitis, candidiasis, hairy leukoplakia, lichen planus reactions, chronic biting, tobacco pouch keratosis, leukoedema, chemical burn, uremic stomatitis, skin graft, some genodermatoses and discoid lupus erythematosus.
Treatment Elimination or discontinuation of predisposing factors, systemic retinoid compounds. Surgical excision is the treatment of choice.
 |
| Homogeneous leukoplakia. |
 |
| Speckled leukoplakia |
Hairy Leukoplakia
Definition Hairy leukoplakia is one of the most common and characteristic lesions of human immunodeficiency virus (HIV) infection. Rarely, it can also appear in immunosuppressed patients after organ transplantation.
Etiology Epstein–Barr virus seems to play an important role in the pathogenesis.
Clinical features Hairy leukoplakia presents as a white asymptomatic, often elevated and unremovable patch. The lesion is almost always found bilaterally on the lateral margins of the tongue, and may spread to the dorsumand the ventral surface. Characteristically, the surface of the lesion is corrugated with a vertical orientation. However, smooth and flat lesions may also be seen. The lesion is not precancerous.
Laboratory tests Histological examination, in situ hybridization, polymerase chain reaction (PCR) and electron microscopy.
Differential diagnosis Chronic biting, lichen planus, frictional keratosis, cinnamon contact stomatitis, uremic stomatitis, candidiasis.
Treatment Not required; however, in some cases aciclovir or valaciclovir can be used with success.
 |
| Hairy leukoplakia. |
Lichen Planus
Definition Lichen planus is a relatively common chronic inflammatory disease of the oral mucosa and skin.
Etiology Although the cause is not well known, T cell-mediated autoimmune phenomena are involved in the pathogenesis of lichen planus.
Clinical features White papules that usually coalesce, forming a network of lines (Wickman’s striae), are the characteristic oral lesions of the disease. Six forms of the disease are recognized in the oral mucosa, classified according to frequency: the common ;the less common ; and the rare . Middle-aged individuals are more com-monly affected (the ratio of women to men ratio is 3 : 2). The buccal mucosa, tongue, and gingiva are the sites of predilection. The skin lesions characteristically appear as polygonal purple, pruritic papules, usually affecting the flexor surfaces of the extremities. The glans penis and nails may also be affected. The disease can usually be diagnosed on clinical grounds alone. The prognosis of lichen planus is usually good, and malignant transformation (particularly of the erosive form) remains controversial.
Laboratory tests Histopathological examination is very helpful. Direct immunofluorescence can also be used, although the features are not specific.
Differential diagnosis Discoid lupus erythematosus, candidiasis, graft-versus-host disease, geographic tongue, leukoplakia, erythroplakia, cicatricial pemphigoid, pemphigus, bullous pemphigoid.
Treatment No treatment is needed in asymptomatic lesions. Topical steroids (ointment in Orabase, intralesional injection), may be helpful. Systemic steroids in low doses can be used in severe and extensive cases. The topical use of antiseptic mouthwashes should be avoided.
 |
| Lichen planus of the buccal mucosa: reticular form. |
 |
| Lichen planus of the dorsum of the tongue: hypertrophic form. |
 |
| Lichen planus, papular and reticular forms, of the buccal mucosa |
 |
| Lichen planus, pigmented form, of the buccal mucosa |
Lichenoid Reactions
Definition Lichenoid or lichen planus reactions are a heterogeneous group of lesions of the oral mucosa that show clinical and histopathological similarities to lichen planus, but have a different course.
Etiology Hypersensitivity to dental restorative materials, amalgam, composite resins and dental plaque accumulation are the most common causative factors. Rarely, a reaction to drugs may be responsible.
Clinical features Clinically, they appear as white and/or erythematous lesions, usually associated with peripheral delicate white striae.
Erosions are also common . The lesions mimic erosive lichen planus. Characteristically, the lesions are strictly confined to the mucosa directly in contact with the restorative materials, and do not migrate to other sites. The lesions disappear after removal of the adjacent material.
The diagnosis is usually made clinically.
Laboratory tests A skin punch test may be helpful in some cases.
Differential diagnosis Lichen planus, fixed drug eruption, discoid lupus erythematosus, cicatricial pemphigoid, cinnamon contact stomatitis.
Treatment Replacement of the restorative material, polishing and smoothing, and good oral hygiene are recommended. Topical steroid treatment for a short time is also helpful.
 |
| Lichanoid drug reaction to allopurinol: white hyperkeratotic lesions and superficial erosions on the sides of the tongue. |
 |
| Lichenoid reaction to dental amalgam and cold: white and erythematous lesions on the buccal mucosa |
Linea Alba
Definition Linea alba is a relatively common alteration of the buccal mucosa.
Etiology Pressure, sucking fromthe buccal surface of the teeth.
Clinical features It presents as an asymptomatic, bilateral, linear elevation with a slightly whitish color at the level of the occlusal line of the teeth. It has a normal consistency on palpation. The diagnosis is based on clinical grounds alone.
Treatment No treatment is required.
 |
| Linea alba. |
Nicotinic Stomatitis
Definition Nicotinic stomatitis, or smoker’s palate, is a common tobacco- related type of keratosis that occurs exclusively on the hard palate, and is classically associated with heavy pipe and cigar smoking.
Etiology The elevated temperature, rather than the tobacco chemicals, is responsible for this lesion.
Clinical features Clinically, the palatal mucosa initially responds to the high temperature with redness. Later, it becomes wrinkled and takes on a diffusely grayish-white color, with numerous micronodules with characteristic punctate red centers, which represent the inflamed and dilated orifices of the minor salivary gland ducts. The lesions are not premalignant, in contrast to the “reverse smoker’s palate” lesion, which is associated with reverse smoking.
Laboratory tests Usually not required. However, a histopathological examination is useful.
Differential diagnosis Reverse smoker’s palate, leukoplakia, discoid lupus erythematosus, candidiasis, lichen planus.
Treatment Cessation of smoking.
 |
| Nicotinic Stomatitis |
Uremic Stomatitis
Definition Uremic stomatitis is a rare disorder that may occur in patients with acute or chronic renal failure.
Etiology Increased concentration of urea and its products in the blood and saliva. The pathogenesis of oral lesions is not clear. It usually appears when blood concentration of urea exceeds 30 mmol/1. The degradation of oral urea by the enzyme urease forms free ammonia, which may damage the oral mucosa.
Clinical features Four forms of uremic stomatitis are recognized: (a) the ulcerative form, (b) the hemorrhagic form, (c) the nonulcerative, pseudomembranous form, and (d) the hyperkeratotic form. The last two forms appear as white lesions. The nonulcerative, pseudomembranous form presents as painful diffuse erythema covered by a thick whitish-gray pseudomembrane. The hyperkeratotic formpresents asmultiple painful white hyperkeratotic lesions with thin projections. The tongue, and the floor of the mouth are more frequently affected. Xerostomia, uriniferous breath odor, unpleasant taste, and a burning sensation are common symptoms. Candidiasis and viral and bacterial infections are common oral complications. The diagnosis is based on the history, the clinical features, urinalysis and blood urea level determination.
Differential diagnosis Candidiasis, cinnamon contact stomatitis, hairy leukoplakia, white sponge nevus, drug reactions.
Treatment The oral lesions usually improve after hemodialysis. A high level of oral hygiene, mouthwashes with oxygen release agents, and artificial saliva are suggested. Antimycotic, antiviral, and antimicrobial agents if necessary.
 |
| Uremic stomatitis, white hyperkeratotic lesions mimic hairy leukoplakia on the lateral border of the tongue |
 |
| Uremic stomatitis, whitish-gray pseudomembranes on the tongue and floor of the mouth. |
Cinnamon Contact Stomatitis
Definition Cinnamon contact stomatitis is a relatively common oral mucosal reaction to continuous contact of substances with cinnamon.
Etiology Artificial cinnamon flavoring especially in the form of chewing gum, candies, toothpaste, drops, etc.
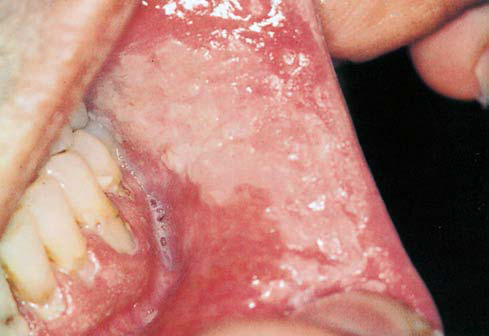
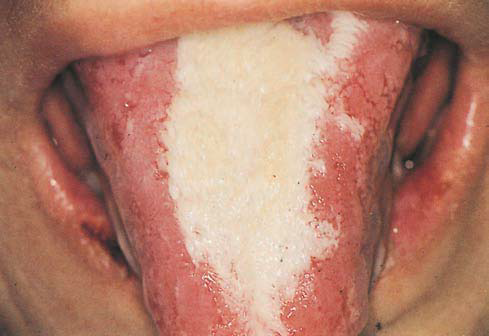
Clinical features The condition is characterized by erythema of the oral mucosa, usually in association with desquamation and erosions. White hyperkeratotic plaques are very common. A burning sensation and pain are common symptoms. The lateral borders of the tongue, the buccal mucosa, and the gingiva are more frequently affected. Exfoliative cheilitis and perioral dermatitis may occur. The diagnosis is based on the history and the clinical features.
Differential diagnosis Amalgam contact stomatitis, chronic biting, leukoedema, epithelial peeling, hairy leukoplakia, leukoplakia, candidiasis, uremic stomatitis, lichen planus, discoid lupus erythematosus.
Treatment Discontinuation of any cinnamon product improves the signs and symptoms in approximately two weeks. In severe and extended lesions with erosions, low doses of steroids (e.g., 10 mg/day prednisolone) for one week help the lesions to heal.
 |
| Cinnamon Contact Stomatitis |
 |
| Cinnamon Contact Stomatitis |
Chemical Burn
Definition This is an injury to the oral mucosa caused by topical application of caustic agents.
Etiology Causative agents include aspirin, hydrogen peroxide, phenol, alcohol, sodiumperb orate, silver nitrate, trichloroacetic acid, acid etching liquid, and varnishes of tooth cavities.
Clinical features Clinically, the affected mucosa is covered with a white membrane due to necrosis. The necrotic epitheliumcan easily be scraped off, leaving a red, bleeding surface. The lesions are painful. The diagnosis should be made on the basis of the clinical features and history.
Differential diagnosis Necrotizing ulcerative gingivitis and stomatitis, materia alba, candidiasis, mechanical trauma, bullous diseases.
Treatment Treatment is symptomatic.
 |
| Aspirin Burn |
 |
| Phenol burn |
 |
| Trichloroacetic acid burn |
Candidiasis
Definition Candidiasis is the most common oral fungal infection. Over the last two decades, the disease has taken on major importance.
Etiology It is usually caused by Candida albicans, and less frequently by other fungal species (C. glabrata, C. krusei, C. tropicalis, C. parapsilosis). Predisposing factors are local (poor oral hygiene, xerostomia, mucosal damage, dentures, antibiotic mouthwashes) and systemic (broad-spectrum antibiotics, steroids, immunosuppressive drugs, radiation, HIV infection, hematological malignancies, neutropenia, iron-deficiency anemia, cellular immunodeficiency, endocrine disorders).
Clinical features Oral candidiasis is classified as primary, consisting of lesions exclusively on the oral and perioral area, and secondary, consisting of oral lesions of mucocutaneous disease. Primary candidiasis includes five clinical varieties: pseudomembranous, erythematous, nodular, papillary hyperplasia of the palate, and Candida-associated lesions (angular cheilitis, median rhomboid glossitis, denture stomatitis). The main forms of candidiasis that produce white lesions are the following.
Pseudomembranous candidiasis is the most common form of the disease, and is clinically characterized by creamy-white, slightly elevated, removable spots or plaques. The lesions may be localized or generalized, and appear more frequently on the buccal mucosa, soft palate, tongue, and lips. Xerostomia, a burning sensation, and an unpleasant taste are the most common symptoms.
 |
| Pseudomembranous candidiasis |
 | |||||||
| Nodular candidiasis |
 |
| Nodular candidiasis |
Nodular candidiasis is a chronic formof the disease; it appears clinically as a white, firm, and raised plaque that usually does not detach.
Mucocutaneous candidiasis is a heterogeneous and rare group of clinical syndromes, characterized by chronic lesions of the skin, nails, and mucosae, and usually associated with immunological defects. Clinically, the oral lesions appear as white and usually multiple plaques, which cannot be removed.
Laboratory tests Cytology and tissue culture examination; biopsy only in chronic cases.
Differential diagnosis Leukoplakia, hairy leukoplakia, lichen planus, syphilitic mucous
patches, white sponge nevus, chemical and traumatic lesions, cinnamon contact stomatitis, lupus erythematosus.
Treatment Topical antifungal agents (nystatin, azole derivatives, amphotericin B). Systemic azoles (ketoconazole, fluconazole, itraconazole).
Chronic Biting
Definition and etiology Mild chronic biting of the oral mucosa is relatively common in nervous individuals. These patients consciously bite the buccal mucosa, lips, and tongue, and detach the superficial epithelial layers.
Clinical features The lesions are characterized by a diffuse irregular white area of small furrows and desquamation of the epithelium. Rarely, erosions and petechiae may be seen. The diagnosis is made clinically.
Differential diagnosis Candidiasis, lichen planus, leukoplakia, hairy leukoplakia, white sponge nevus, leukoedema, cinnamon contact stomatitis.
Treatment Recommendation to stop the habit.
Definition Geographic tongue, or erythema migrans, is a relatively common benign condition, primarily affecting the tongue and rarely other oral mucosa sites (geographic stomatitis)
Etiology The exact etiology remains unknown. It may be genetic.
Clinical features Clinically, the condition is characterized by multiple, well-demarcated, erythematous, depapillated patches, typically surrounded by a slightly elevated whitish border, and usually restricted to the dorsumof the tongue. Characteristically, the lesions persist for a short time in one area, then disappear completely and reappear in another area. The condition is usually asymptomatic, and often coexists with fissured tongue. The diagnosis is made clinically.
Differential diagnosis Candidiasis, lichen planus, psoriasis, Reiter syndrome,
syphilitic mucous patches.
Treatment Reassurance of the patient.
 |
| Geographic tongue |
 |
| Geographic tongue-Localized lesion |
 |
| Geographic tongue with prominent whitish border |
Hairy Tongue
Definition Hairy tongue is a relatively common disorder that is due to marked accumulation of keratin on the filiform papillae of the tongue, resulting in a hairlike pattern.
Etiology Unknown. Predisposing factors are poor oral hygiene, oxidizing mouthwashes, antibiotics, excessive smoking, radiation therapy, emotional stress, and bacterial and Candida species infections.
Clinical features Clinically, it is characterized by an asymptomatic elongation of the filiformpapillae of the dorsum of the tongue, sometimes extending over several millimeters. The color may range from whitish to brown or black. The diagnosis is made clinically.
Treatment Elimination of predisposing factors, brushing of the tongue,local use of keratolytic agents (trichloroacetic acid, podophyllin).
 |
| Hairy tongue |
 |
| Hairy tongue |
 |
| Hairy tongue |
Furred Tongue
Definition Furred tongue is a relatively uncommon disorder, usually appearing during febrile illnesses.
Etiology The cause is not clear. Predisposing factors are febrile painful oral lesions, poor oral hygiene, dehydration, and soft diet.
Clinical features Clinically, it appears as a white or whitish-yellow thick coating on the dorsal surface of the tongue . The lesion is due to lengthening of the filiformpapillae, by up to 3–4 mm, and accumulation of debris and bacteria. Characteristically, furred tongue appears and disappears within a short period. The diagnosis is made clinically.
Differential diagnosis Hairy tongue, hairy leukoplakia, candidiasis.
Treatment Therapy of the underlying illnesses and improvement of oral hygiene.
Definition and etiology Materia alba results fromthe accumulation of food debris, dead epithelial cells, and bacteria. It is common at the dentogingival margin. Rarely, materia alba may be seen along the vestibular surface of the attached gingiva in patients with poor oral hygiene.
Clinical features It presents as a soft, whitish plaque that is easily detached after slight pressure.
Differential diagnosis Candidiasis, chemical burn, leukoplakia.
Treatment Good oral hygiene
 |
| White plaques on the attached gingiva and the alveolar mucosa, caused by materia alba accumulation |
Fordyce’s Granules
Definition Fordyce’s granules are ectopic sebaceous glands of the oral mucosa.
Etiology It is a normal anatomical variation.
Clinical features Clinically, the granules present as multiple, asymptomatic, slightly raised whitish-yellow spots. The vermilion border of the upper lip, the commissures, and the buccal mucosa are the sites of predilection. They occur in about 80% of adults of both sexes. The diagnosis is based on the clinical features alone.
Differential diagnosis Lichen planus, leukoplakia, candidiasis.
Definition Leukoedema is a normal anatomical variation.
Etiology It is due to increased thickness of the epitheliumand intracellular edema of the prickle-cell layer.
Clinical features Clinically, it is characterized by a grayish-white, opalescent pattern of the mucosa and a slightly wrinkled surface, which characteristically disappears when the mucosa is everted and stretched. It usually occurs bilaterally on the buccal mucosa, and rarely on the tongue and lips.
Differential diagnosis Leukoplakia, hairy leukoplakia, lichen planus.
White Sponge Nevus
Definition White sponge nevus, or Cannon disease, is a relatively rare genodermatosis.
Etiology Genetic. It is inherited as an autosomal dominant trait.
Clinical features It presents as symmetrical white lesions with multiple furrows and a spongy texture. The lesions may appear at birth, or more commonly in early childhood. The buccal mucosa and the ventral surface of the tongue are the sites of predilection, although lesions may develop anywhere in the mouth, or even in the vaginal and rectal mucosa.
Laboratory tests Histopathological examination.
Differential diagnosis Leukoedema, leukoplakia, lichen planus, chronic biting, dyskeratosis congenita, pachyonychia congenita.
Treatment No treatment is required.
Definition Dyskeratosis congenita, or Zinsser–Engman–Cole syndrome, is an uncommon disorder.
Etiology Genetic. It is probably inherited as a recessive autosomal and X-linked trait.
Clinical features It is characterized by hyperpigmentation, atrophic skin areas, telangiectasia, nail dystrophy, hyperhidrosis, skin and mucosal bullae, blepharitis and ectropion, anemia, and oral manifestations. The oral lesions consist of recurrent blisters, epithelial atrophy, and leukoplakia. Squamous-cell carcinoma may occur.
Differential diagnosis Leukoplakia, lichen planus, epidermolysis bullosa,
pachyonychia congenita.
Definition Pachyonychia congenita, or Jadassohn–Lewandowski syndrome, is an uncommon genodermatosis.
Etiology Genetic. It is inherited as an autosomal dominant trait.
Clinical features It is characterized by symmetrical nail thickening, palmoplantar hyperkeratosis, hyperhidrosis, blister formation, follicular keratosis, and oral lesions. The oral lesions appear at birth or shortly afterward, and present as thick and white or grayish-white plaques, usually on the buccal mucosa, the tongue, and the gingiva. The diagnosis is based on the history and the clinical features.
Differential diagnosis Dyskeratosis congenita, leukoplakia, lichen planus, white sponge nevus, and focal palmoplantar and oral mucosa hyperkeratosis syndrome.
Treatment Supportive.
 |
| Focal palmoplantar hyperkeratosis |
 |
| Pachyonychia congenita: grayish-white lesion on the buccal mucosa |
Focal Palmoplantar and Oral Mucosa Hyperkeratosis Syndrome
Definition This is a rare mucocutaneous disorder.
Etiology Genetic. It is inherited as an autosomal dominant trait.
Clinical features The main clinical manifestations are focal hyperkeratosis on the weight-bearing and pressure-related regions of the palms, soles, and oral mucosa. Rarely, thickening of the nails and hyperhidrosis may be seen. The oral lesions present as white hyperkeratotic plaques (leukoplakia), mainly on the attached gingiva, the lateral border of the tongue, and the palate. The lesions usually develop in early childhood.
Differential diagnosis Pachyonychia congenita, dyskeratosis congenita, leukoplakia.
Treatment Supportive. Retinoids may be helpful.
 |
| Focal Palmoplantar and Oral Mucosa Hyperkeratosis Syndrome |
Papilloma
Papilloma appears as an exophytic, painless, usually pedunculated growth. Characteristically, the tumor has a white or normal color, with numerous fingerlike projections that form a cauliflower pattern. Papilloma is usually solitary, with a size of 0.5–1 cm.
 |
| Papilloma on Buccal Mucosa |
Verrucous Carcinoma
Definition Verrucous carcinoma is a low-grade variant of squamouscell
carcinoma.
Etiology Human papillomavirus is presumably involved in the pathogenesis.
Clinical features Clinically, it presents as an exophytic white mass with a verrucous or pebbly surface. The size varies from1 cm in the early stages to very extensive lesions. The buccal mucosa, palate, and alveolar mucosa are the most common sites of involvement. Verrucous carcinoma mainly develops in smokers over 60 years of age.
Laboratory tests Histopathological examination.
Differential diagnosis Verrucous leukoplakia, papilloma, verruciform xanthoma, white sponge nevus, squamous-cell carcinoma.
Squamous-Cell Carcinoma
Squamous-cell carcinoma has a wide spectrum of clinical features. In about 5–8% of cases, it appears in the early stages as a white asymptomatic plaque identical to leukoplakia. Biopsy and histopathological examination are important for the diagnosis in these cases.
Skin and Mucosal Grafts
Definition Skin and mucosal grafts are often utilized in the oral cavity to cover mucosal defects after extensive surgery for benign and malignant tumors, or as free gingival graft.
Clinical features clinically, both forms of grafts (skin and mucosal) usually present as a whitish, or gray-white plaque. The size of the plaque depends on the size of the graft. Occasionally, the color of the skin graft is black, due to melanin overproduction. If the graft contain hair follicles, hairs may develop in the oral cavity. The tongue, buccal mucosa, palate, gingiva and alveolar mucosa are the most common sites where skin and mucosal grafts are placed. Skin graft into the oral cavity may be associated with unpleasant feelings. The diagnosis is based on the history and the clinical features.
Differential diagnosis Leukoplakia, traumatic scar, epidermolysis bullosa.
Epithelial Peeling
Definition Epithelial peeling is a relatively common superficial desquamation
(epitheliolysis) of the oral mucosa.
Etiology It is caused by the direct irritating effect of toothpastes that contain sodium lauryl sulfate or pyrophosphates. The same phenomenon may be associated with chlorhexidine mouthwash. Sometimes the lesions are idiopathic.
Clinical features Clinically, epithelial peeling presents as superficial painless white plaques or dots that can be easily lifted fromthe oral mucosa. The buccal mucosa, lip mucosa, and mucobuccal and mucolabial folds are more frequently affected. The lesions usually disappear when the individual stops using these toothpastes or mouthwashes. The diagnosis is based entirely on the history and the clinical features.
Differential diagnosis Chemical burn, chronic biting, candidiasis, leukoplakia.









It is no secret that I have a very deep and personal relationship with God. I have pushed and resisted that relationship this past year through all the bullshit I have had to go through living with Herpes but once again, God is bigger than my stubbornness and broke through that outbreak cold sore and all I had Genital Herpes. For me personally, hearing over and over how I am not good enough has really invaded my mind in the worst way possible. I completely shut down and I was just waking up like is this how life going to end this temporary herpes outbreak “fuck everybody with herpes if you know what I mean” but let's be honest here...
BalasHapusIt is a cowardly to say no to herbal medicine. It is fear based. And it is dishonest to what my heart wants. Don't build a wall around yourself because you are afraid of herbals made or taking a bold step especially when it's come to health issues and getting cure. So many young men/ women tell me over and over that Dr Itua is going to scam me but I give him a try to today I feel like no one will ever convince me about herbal medicine I accept Dr Itua herbal medicine because it's cure my herpes just two weeks of drinking it and i have been living for a year and months now I experience outbreak no more, You can contact him if you need his herbal medicine for any such diseases like, Herpes, Schizophrenia,Cancer,Scoliosis,Fibromyalgia,Fluoroquinolone Toxicity Syndrome Fibrodysplasia Ossificans Progressiva.Fatal Familial Insomnia Factor V Leiden Mutation ,Epilepsy Dupuytren's disease,Desmoplastic,Diabetes ,Coeliac disease,Creutzfeldt–Jakob,Dairies,Lyme Disease,Epilepsy, ,ALS,Hepatitis,Copd,Parkinson disease.Genetic disease,Fibrodysplasia disease,Fibrodysplasia Ossificans Men/Woman infertility, bowel disease ,Huntington's disease ,Diabetes,Fibroid. disease,Lupus,Lipoid Storage diseases( Gauchers disease),Polycystic Disease.,Cerebral Amyloid Angiopathy, Ataxia,Cirrhosis of Liver,Arthritis,Amyotrophic Lateral Sclerosis,Alzheimer's disease,Adrenocortical carcinoma.Asthma,Allergic,HIV, Epilepsy, Infertility, Love Spell,. Email..drituaherbalcenter@gmail.com then what's app.+2348149277967.... My advice to any sick men/women out there is simple... Be Always an open book. Be gut wrenching honest about yourself, your situation, and what you are all about. Don't hold anything back. Holding back will get you nowhere...maybe a one way ticket to lonelyville and that is NOT somewhere you want to be. So my final truth...and I'm just starting to grasp this one..