
Premature eruption, natal, and neonatal teeth
Teeth erupted at birth (natal teeth) or which erupt within the first 30 days of life (neonatal teeth) are uncommon, occurring in about 1 in 3000 live births in most reported series. In about 80 per cent of cases the mandibular incisors, usually one or both central incisors, are involved. They are thought to arise from normal tooth germs developing in a superficial position in the jaw with subsequent premature eruption. Coronal enamel and dentine formation is normal for the chronological age of the tooth, but because of the premature eruption the enamel may be hypoplastic. However, there is usually a virtual absence of root formation and any radicular dentine or cementum that forms is generally irregular in structure due to the mobility of the tooth in the jaw (Such teeth may be lost spontaneously or have to be extracted if there is a risk of dislocation and inhalation, or if they interfere with feeding.
Premature eruption of other deciduous or permanent teeth is rare and may be related to local factors such as a superficial location of a tooth germ or early shedding of deciduous teeth. Generalized early eruption of the permanent dentition may also be seen in children with endocrine abnormalities associated with an excess secretion of growth hormone or with hyperthyroidism.
Retarded eruption
Endocrinopathies (for example hypothyroidism), prematurity, nutritional deficiencies, and chromosome abnormalities, such as Down syndrome, may very occasionally be associated with retarded eruption of either the deciduous and/or permanent dentition. Idiopathic migration, traumatic displacement of tooth germs, or abnormally large crowns may also be associated with retarded eruption. Delayed eruption and multiple, impacted supernumerary teeth are also a feature of cleidocranial dysplasia
Premature loss
This is usually the result of either dental caries and its sequelae, or chronic periodontal disease. Occasionally, premature loss of teeth is more specifically associated with diseases such as hypophosphatasia, hereditary palmar-plantar hyperkeratosis, and other causes of periodontitis in systemic disease.
Persistence of deciduous teeth
This occurs when deciduous teeth are not shed at the expected time, and is usually associated with the failure of eruption of the permanent successor because it is missing or displaced. Persistence of the entire deciduous dentition is uncommon and usually has a systemic background, such as cleidocranial dysplasia when eruption of permanent teeth is impeded.
Impaction of teeth
An impacted tooth is one which remains unerupted, or only partly erupted, in the jaw beyond the time when it should normally be fully erupted. One or several teeth may be affected and the condition may be symmetrical. It is rarely seen in the primary dentition. In the permanent dentition the teeth most frequently involved are third molars, mandibular premolars, and maxillary canines. Local causes for impaction include abnormal position of the tooth germ, lack of space for the teeth in the jaws, supernumerary teeth, cysts, and tumours. As previously mentioned, cleidocranial dysplasia is almost always associated with multiple impacted teeth. Possible complications of impaction include resorption of the impacted tooth or adjacent erupted teeth, and the development of dentigerous cysts and odontogenic tumours.
Reimpaction of teeth
This term describes the situation in which a previously erupted tooth becomes submerged in the tissues. Alternative terms for the disorder are infraocclusion and submerged teeth. The deciduous second molar is most commonly affected and reimpaction occurs twice as frequently in the mandible than in the maxilla.The condition is associated with deficient development of the alveolar process around the reimpacted tooth which may, on rare occasions, become completely covered by oral mucosa. The roots of the tooth are usually partly resorbed and ankylosed to the bone. The cause is not known, but it is likely that the root first becomes ankylosed and that this is followed by lack of growth of the alveolar process. As the neighbouring teeth continue to move occlusally they tilt over the ankylosed tooth, causing reimpaction.
Endocrinopathies (for example hypothyroidism), prematurity, nutritional deficiencies, and chromosome abnormalities, such as Down syndrome, may very occasionally be associated with retarded eruption of either the deciduous and/or permanent dentition. Idiopathic migration, traumatic displacement of tooth germs, or abnormally large crowns may also be associated with retarded eruption. Delayed eruption and multiple, impacted supernumerary teeth are also a feature of cleidocranial dysplasia
Premature loss
This is usually the result of either dental caries and its sequelae, or chronic periodontal disease. Occasionally, premature loss of teeth is more specifically associated with diseases such as hypophosphatasia, hereditary palmar-plantar hyperkeratosis, and other causes of periodontitis in systemic disease.
Persistence of deciduous teeth
This occurs when deciduous teeth are not shed at the expected time, and is usually associated with the failure of eruption of the permanent successor because it is missing or displaced. Persistence of the entire deciduous dentition is uncommon and usually has a systemic background, such as cleidocranial dysplasia when eruption of permanent teeth is impeded.
Impaction of teeth
An impacted tooth is one which remains unerupted, or only partly erupted, in the jaw beyond the time when it should normally be fully erupted. One or several teeth may be affected and the condition may be symmetrical. It is rarely seen in the primary dentition. In the permanent dentition the teeth most frequently involved are third molars, mandibular premolars, and maxillary canines. Local causes for impaction include abnormal position of the tooth germ, lack of space for the teeth in the jaws, supernumerary teeth, cysts, and tumours. As previously mentioned, cleidocranial dysplasia is almost always associated with multiple impacted teeth. Possible complications of impaction include resorption of the impacted tooth or adjacent erupted teeth, and the development of dentigerous cysts and odontogenic tumours.
Reimpaction of teeth
This term describes the situation in which a previously erupted tooth becomes submerged in the tissues. Alternative terms for the disorder are infraocclusion and submerged teeth. The deciduous second molar is most commonly affected and reimpaction occurs twice as frequently in the mandible than in the maxilla.The condition is associated with deficient development of the alveolar process around the reimpacted tooth which may, on rare occasions, become completely covered by oral mucosa. The roots of the tooth are usually partly resorbed and ankylosed to the bone. The cause is not known, but it is likely that the root first becomes ankylosed and that this is followed by lack of growth of the alveolar process. As the neighbouring teeth continue to move occlusally they tilt over the ankylosed tooth, causing reimpaction.
Non-bacterial loss of tooth substance
Introduction
Although it is convenient to discuss attrition, abrasion, and erosion separately, in many patients tooth wear involves elements of all three. For this reason terms such as 'tooth wear with a major component of attrition' are usually preferred as clinical diagnoses.
Key points - Non-bacterial loss of tooth substance
· tooth wear
- attrition
- abrasion
- erosion
· resorption
- internal
- external
Attrition
Introduction
Although it is convenient to discuss attrition, abrasion, and erosion separately, in many patients tooth wear involves elements of all three. For this reason terms such as 'tooth wear with a major component of attrition' are usually preferred as clinical diagnoses.
Key points - Non-bacterial loss of tooth substance
· tooth wear
- attrition
- abrasion
- erosion
· resorption
- internal
- external
Attrition

This is loss of tooth substance as a result of tooth-to-tooth contact (Fig. 3.3). It may be physiological or pathological in origin, although clinically the distinction is often unclear. The pattern of tooth loss in physiological attrition is fairly constant: the incisal edges of the incisors are worn first, followed by the occlusal surfaces of the molars, the palatal cusps of the maxillary teeth, and the buccal cusps of the mandibular teeth. When the dentine becomes exposed it generally becomes discoloured brown. Because dentine is softer than enamel it is attrited at a greater rate and the lesions may become cup-shaped, surrounded by a rim of enamel. Approximal attrition leads to the transformation of contact points to contact areas and to the mesial migration of teeth which throughout life may amount to as much as 1cm from third molar to third molar. Men generally show more severe attrition than women. The abrasive property of food is important in determining the rate of physiological attrition.
Pathological attrition may result from:
(1) abnormal occlusion - either developmental or following extractions;
(2) bruxism and habits such as tobacco and betel chewing;
(3) abnormal tooth structure, for example amelogenesis imperfecta, dentinogenesis imperfecta.
Exposure of dentinal tubules by attrition leads to the formation of reactionary dentine on the pulpal surface which protects the tooth against pulp exposure, and to the formation of translucent zones and dead tracts. The patient may complain of hypersensitive dentine.

This is the pathological wearing away of tooth substance by the friction of a foreign body independent of occlusion. Different foreign bodies produce different patterns of abrasion.
1. Toothbrush abrasion is common and is seen most frequently on exposed root surfaces of teeth. It is commonly associated with toothbrushing in a horizontal rather than a vertical direction and is made worse by an abrasive dentifrice. The maxillary teeth are more involved than the mandibular teeth, and the abrasion is most pronounced in the cervical regions of the labial surfaces of incisors, canines, and premolars. The abrasion produces wedge-shaped grooves with sharp angles and highly polished dentine surfaces. Abrasion cavities may be accentuated as a result of flexing of the teeth due to excessive loading, such as in a traumatic occlusion. This can cause microcracks in the enamel, termed abfraction lesions.
2. Habitual abrasion may be seen in pipe-smokers.
3. Occupational abrasion develops when objects are held between or against the teeth during work, for example hair-grips.
4. Ritual abrasion of the teeth is uncommon today and is confined mainly to Africa.
Erosion

This is the loss of tooth substance by a chemical process that does not involve known bacterial action. It may render the teeth more susceptible to attrition and abrasion.
1. Dietary erosion may follow the excessive intake of acidic beverages, such as fruit juices or carbonated soft drinks, or the habit of sucking citrus fruits. Although the cause of erosion cannot be reliably determined from the distribution of the lesions, dietary erosions tend to involve the palatal surfaces of the teeth and the labial surfaces of the maxillary incisors. It is a common problem, occurring to some extent in about 50 per cent of 5-year-old and about 30 per cent of 14-year-old children in the UK. Shallow, broad concavities with polished surfaces are produced.
2. Occupational (environmental) erosion is now relatively uncommon. It is seen in workers exposed to acids in their workplace and is usually due to atmospheric pollution. The labial surfaces of the maxillary and mandibular incisors are usually involved as these are the surfaces most exposed to the atmosphere.
3. Regurgitation of stomach contents or persistent vomiting causes erosion in which the palatal surfaces of the maxillary teeth are primarily affected - a condition referred to as perimolysis. This may be associated with anorexia nervosa or bulimia nervosa. A similar pattern of erosion may also be seen in other patients with gastro-oesophageal reflux, for example chronic alcoholics, where gastric reflux is probably associated with chronic gastritis.
As in attrition, reactionary dentine, translucent zones, and dead tracts develop in relation to the exposed dentinal tubules and the patients may complain of hypersensitive dentine.
Key points - Tooth wear
· embraces attrition, abrasion, and erosion alone and in combinations
· combined aetiologies modify clinical patterns of wear
· stimulates protective responses of pulpodentinal complex

This is the loss of tooth substance by a chemical process that does not involve known bacterial action. It may render the teeth more susceptible to attrition and abrasion.
1. Dietary erosion may follow the excessive intake of acidic beverages, such as fruit juices or carbonated soft drinks, or the habit of sucking citrus fruits. Although the cause of erosion cannot be reliably determined from the distribution of the lesions, dietary erosions tend to involve the palatal surfaces of the teeth and the labial surfaces of the maxillary incisors. It is a common problem, occurring to some extent in about 50 per cent of 5-year-old and about 30 per cent of 14-year-old children in the UK. Shallow, broad concavities with polished surfaces are produced.
2. Occupational (environmental) erosion is now relatively uncommon. It is seen in workers exposed to acids in their workplace and is usually due to atmospheric pollution. The labial surfaces of the maxillary and mandibular incisors are usually involved as these are the surfaces most exposed to the atmosphere.
3. Regurgitation of stomach contents or persistent vomiting causes erosion in which the palatal surfaces of the maxillary teeth are primarily affected - a condition referred to as perimolysis. This may be associated with anorexia nervosa or bulimia nervosa. A similar pattern of erosion may also be seen in other patients with gastro-oesophageal reflux, for example chronic alcoholics, where gastric reflux is probably associated with chronic gastritis.
As in attrition, reactionary dentine, translucent zones, and dead tracts develop in relation to the exposed dentinal tubules and the patients may complain of hypersensitive dentine.
Key points - Tooth wear
· embraces attrition, abrasion, and erosion alone and in combinations
· combined aetiologies modify clinical patterns of wear
· stimulates protective responses of pulpodentinal complex
Resorption
The natural shedding of deciduous teeth follows the progressive resorption of the roots by cells resembling osteoclasts. This physiological resorption may be an inherent developmental process or it may be related to pressure from the permanent successor against the overlying bone or tooth.
Microscopic areas of superficial (surface) resorption of the roots of permanent teeth are common but are transient and are repaired by the apposition of cementum or of a bone-like tissue. Such microscopic foci are of no clinical consequence. In contrast, resorption sufficient to be diagnosed radiologically is always pathological. Pathological resorption may start from the root surface (external resorption) or from the pulpal surface (internal resorption). In both cases osteoclast-like giant cells (sometimes called odontoclasts) sitting in resorption lacunae are seen on actively resorbing surfaces. However, as resorption is not a continuous process the osteoclast-like cells are not always present and in this case some resorption lacunae may show attempts at repair.
External resorption
External resorption may be caused by inflammation and by pressure/mechanical stimulation or be of unknown (indiopathic) cause.
INFLAMMATORY RESORPTION
Inflammatory resorption typically involves the apical portion of the root, as a result of periapical inflammation following pulp necrosis or trauma, and is associated with a periapical radiolucency on a radiograph. However, following luxation injuries and reimplantation or transplantation of teeth, a replacement pattern of resorption may be seen. This is characterized by progressive resorption of the root and replacement of the resorbed area by bone. However, there is no ankylosis and there is a zone of inflamed granulation or fibrous tissue of varying extent between the root and bone surfaces. Inflammation may also play a role in pressure/mechanical root resorption and in the burrowing type of external resorption involving the cervical areas of the teeth. These are considered below.
PRESSURE/MECHANICAL RESORPTION
Root resorption associated with pressure/mechanical stimulation may be seen in patients undergoing orthodontic treatment and can be caused by the application of excessive force. It occurs in the apical region and the resorbed area undergoes repair and remodelling when the cause is removed. It is possible that excess force could cause an aseptic necrosis of the periodontal ligament, followed by inflammation. Pressure may also be a factor in root resorption associated with tumours or, occasionally, cysts involving the roots of teeth. However, in both cases, it is likely that cytokines associated with bone resorption are also involved.
IDIOPATHIC RESORPTION
A burrowing type of resorption is most commonly seen. A localized area of the root surface is first resorbed, following which the resorption burrows deeply into and ramifies throughout the dentine, producing a labyrinthine network of lacunae and channels. The resorbed tissue is replaced by granulation tissue in which varying amounts of calcified repair tissue and/or bone may form and ankylosis may result.
The circumpulpal dentine and predentine are generally spared and remain as a narrow shell as the resorption encircles the pulp. The pulp remains vital unless exposed by the resorptive process or by fracture of the residual dentine shell. This type of resorption usually starts in the cervical region of the tooth and it has been suggested that trauma to the cementum may trigger the process. As noted above, it is likely that inflammation plays a role.
Internal resorption
Pathological resorption starting from the pulpal surface (internal resorption) is usually associated with pulpitis and follows the loss of odontoblasts and predentine, which might confer some degree of protection. An idiopathic type of internal resorption also occurs in which there is a well-defined, spherical radiolucent area in the dentine continuous with the pulp chamber or root canal. When the coronal dentine is involved the resorption may present clinically as a pink spot due to the vascular pulp tissue being visible through the overlying enamel. Radiological distinction between idiopathic internal and external (burrowing) resorption may be impossible.
Key points - Resorption of teeth
External
· microscopic surface resorption (transient, reversible)
· inflammatory resorption - periapical inflamation, reimplanted/transplanted teeth
· pressure resorption - orthodontics, possibly tumours/cysts
· idiopathic resorption - burrowing (cervical) resorption
External resorption of the crowns of impacted teeth is uncommon. The enamel is normally separated from the surrounding connective tissues by the reduced enamel epithelium, which appears to confer protection. If the epithelium is lost, in total or in part, a burrowing type of external resorption may follow. Again, calcified repair tissue resembling cementum and/or bone may be formed and ankylosis may result.
The natural shedding of deciduous teeth follows the progressive resorption of the roots by cells resembling osteoclasts. This physiological resorption may be an inherent developmental process or it may be related to pressure from the permanent successor against the overlying bone or tooth.
Microscopic areas of superficial (surface) resorption of the roots of permanent teeth are common but are transient and are repaired by the apposition of cementum or of a bone-like tissue. Such microscopic foci are of no clinical consequence. In contrast, resorption sufficient to be diagnosed radiologically is always pathological. Pathological resorption may start from the root surface (external resorption) or from the pulpal surface (internal resorption). In both cases osteoclast-like giant cells (sometimes called odontoclasts) sitting in resorption lacunae are seen on actively resorbing surfaces. However, as resorption is not a continuous process the osteoclast-like cells are not always present and in this case some resorption lacunae may show attempts at repair.
External resorption
External resorption may be caused by inflammation and by pressure/mechanical stimulation or be of unknown (indiopathic) cause.
INFLAMMATORY RESORPTION
Inflammatory resorption typically involves the apical portion of the root, as a result of periapical inflammation following pulp necrosis or trauma, and is associated with a periapical radiolucency on a radiograph. However, following luxation injuries and reimplantation or transplantation of teeth, a replacement pattern of resorption may be seen. This is characterized by progressive resorption of the root and replacement of the resorbed area by bone. However, there is no ankylosis and there is a zone of inflamed granulation or fibrous tissue of varying extent between the root and bone surfaces. Inflammation may also play a role in pressure/mechanical root resorption and in the burrowing type of external resorption involving the cervical areas of the teeth. These are considered below.
PRESSURE/MECHANICAL RESORPTION
Root resorption associated with pressure/mechanical stimulation may be seen in patients undergoing orthodontic treatment and can be caused by the application of excessive force. It occurs in the apical region and the resorbed area undergoes repair and remodelling when the cause is removed. It is possible that excess force could cause an aseptic necrosis of the periodontal ligament, followed by inflammation. Pressure may also be a factor in root resorption associated with tumours or, occasionally, cysts involving the roots of teeth. However, in both cases, it is likely that cytokines associated with bone resorption are also involved.
IDIOPATHIC RESORPTION
A burrowing type of resorption is most commonly seen. A localized area of the root surface is first resorbed, following which the resorption burrows deeply into and ramifies throughout the dentine, producing a labyrinthine network of lacunae and channels. The resorbed tissue is replaced by granulation tissue in which varying amounts of calcified repair tissue and/or bone may form and ankylosis may result.
The circumpulpal dentine and predentine are generally spared and remain as a narrow shell as the resorption encircles the pulp. The pulp remains vital unless exposed by the resorptive process or by fracture of the residual dentine shell. This type of resorption usually starts in the cervical region of the tooth and it has been suggested that trauma to the cementum may trigger the process. As noted above, it is likely that inflammation plays a role.
Internal resorption
Pathological resorption starting from the pulpal surface (internal resorption) is usually associated with pulpitis and follows the loss of odontoblasts and predentine, which might confer some degree of protection. An idiopathic type of internal resorption also occurs in which there is a well-defined, spherical radiolucent area in the dentine continuous with the pulp chamber or root canal. When the coronal dentine is involved the resorption may present clinically as a pink spot due to the vascular pulp tissue being visible through the overlying enamel. Radiological distinction between idiopathic internal and external (burrowing) resorption may be impossible.
Key points - Resorption of teeth
External
· microscopic surface resorption (transient, reversible)
· inflammatory resorption - periapical inflamation, reimplanted/transplanted teeth
· pressure resorption - orthodontics, possibly tumours/cysts
· idiopathic resorption - burrowing (cervical) resorption
External resorption of the crowns of impacted teeth is uncommon. The enamel is normally separated from the surrounding connective tissues by the reduced enamel epithelium, which appears to confer protection. If the epithelium is lost, in total or in part, a burrowing type of external resorption may follow. Again, calcified repair tissue resembling cementum and/or bone may be formed and ankylosis may result.
Discoloration of teeth
Introduction
Normal variation in the colour of teeth must be distinguished from pathological discoloration.
Causes of discoloration
The colour of teeth may be affected by many factors, alone or in combination. The main groups of causes are listed below.
(1) surface deposits (extrinsic staining);
(2) changes in the structure or thickness of the dental hard tissues;
(3) diffusion of pigments into the dental hard tissues after their formation;
(4) incorporation of pigments into the dental hard tissues during their formation.
Extrinsic staining
Introduction
Normal variation in the colour of teeth must be distinguished from pathological discoloration.
Causes of discoloration
The colour of teeth may be affected by many factors, alone or in combination. The main groups of causes are listed below.
(1) surface deposits (extrinsic staining);
(2) changes in the structure or thickness of the dental hard tissues;
(3) diffusion of pigments into the dental hard tissues after their formation;
(4) incorporation of pigments into the dental hard tissues during their formation.
Extrinsic staining

Green, black, brown, or occasionally red or orange deposits may be adsorbed onto tooth surfaces within the salivary pellicle or dental plaque. The stain may be derived from food, drinks, tobacco, and other habits such as betel nut chewing, mouth-rinses and other topical medicaments, or from occupational exposure to metallic salts. Green and black stains are sometimes seen in children on the labial surfaces of upper anterior teeth. It is thought that these are produced by chromogenic bacteria and such children usually have a low caries experience. However, whether or not this is related in some way to the cause of the staining or to other factors is unknown.
Changes in the structure or thickness of dental hard tissues
Abnormally coloured teeth are seen in amelogenesis and dentinogenesis imperfecta, other types of developmentally hypomineralized and hypoplastic enamel, and white spot enamel caries.
Diffusion of pigments into the dental hard tissues after their formation
In addition to discoloration due to intrinsic change in structure, developmentally hypomineralized enamel and carious enamel may take up stains from materials such as food and tobacco and acquire a dark brown colour. Similar stains may diffuse into dentine exposed by caries or tooth wear, and some restorative and root filling materials and their corrosion products may also stain dentine. Pulp necrosis is a common cause of a discoloured tooth. Lysis of necrotic tissue and of red blood cells from areas of haemorrhage leads to pigmented products which diffuse into the dentine.
Incorporation of pigments into the dental hard tissues during their formation
This occurs in congenital disorders associated with hyperbilirubinaemia, congenital porphyria, and tetracycline pigmentation.
CONGENITAL HYPERBILIRUBINAEMIA (NEONATAL JAUNDICE)
Mild transient jaundice is common in neonates but in severe cases, most frequently associated with haemolytic disease of the newborn (rhesus incompatibility), bile pigments may be deposited in the calcifying enamel and dentine of developing teeth, particularly along the neonatal incremental line. The pigment is largely confined to the dentine, the affected teeth being discoloured green to yellowish-brown. Enamel hypoplasia may also occur.
CONGENITAL PORPHYRIA
This is a rare, recessive autosomal disease in which there is an inborn error of porphyrin metabolism. It is characterized by the excretion of red porphyrin pigments in the urine and circulating porphyrins in the blood which are deposited in many tissues, including bone and dental hard tissues. Affected teeth show a pinkish-brown discoloration and a red fluorescence under ultraviolet light.
TETRACYCLINE PIGMENTATION
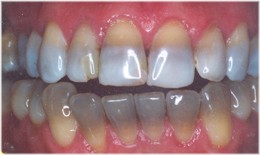
Systemic administration of tetracyclines during the period of tooth development results in their deposition in the dental hard tissues as well as in bone. Dentine is more heavily stained than enamel and in ground sections of affected teeth yellow bands of pigmentation related to incremental lines in dentine can be seen. The pigmented bands fluoresce a bright yellow under ultraviolet light.Tetracyclines are also deposited in cementum.
Affected teeth generally are yellowish when they erupt and become darker and browner after exposure to light. The degree of clinical discoloration of the teeth is affected by which particular tetracycline preparation has been taken, the dosage, and the age of the patient at the time of administration of the drug . If the drug is administered when crown formation is already complete, then the tetracycline is confined to the roots and the discoloration will not be clinically discernible. Tetracyclines cross the placenta and the deciduous teeth may be affected if the drug is given any time from 29 weeks to full term. It is particularly important to avoid tetracyclines from 4 months to about 7 years of age if severe clinical discoloration of the permanent dentition is to be prevented.
Transplantation and reimplantation of teeth
Transplantation of a tooth from one site to another in the same individual (autotransplantation), into an extraction site or a surgically prepared socket, has been carried out for many years with varying degrees of success. Reimplantation is when a tooth is returned to its own socket, usually following traumatic avulsion. Transplantation of teeth from one individual to another of the same species (allografting) has been studied experimentally in animals but the results are very inconsistent because of graft rejection.
Autotransplants do not stimulate an immune response. Experimental studies in animals have shown that following transplantation or reimplantation the pulp and soft tissues attached to the root degenerate due to traumatic severence of the blood supply. In developing teeth with open apices, revascularization and repair of the dental papilla may occur and dentinogenesis may resume, although the dentine formed may be abnormal. However, continued root growth is rare. The reparative cells are probably derived from residual donor tissue which survives operative trauma. Reattachment of autotransplants may result from regeneration of the periodontal ligament, the formation of scar-like fibrous tissue running parallel to the root surface, or ankylosis. If ankylosis occurs the alveolar bone may be directly attached to the normal root surface or to resorption concavities. It has been suggested that preservation of the vitality of the periodontal ligament is an important factor in deterring root resorption and ankylosis.
Clinical studies of autotransplants in humans have concentrated mainly on root resorption which is the most commonly encountered complication. Sometimes the resorption is rapid, but more often is slowly progressive and periods of 10-15 years may elapse before resorption causes exfoliation of the transplanted tooth. Root resorption may be extensive before marked tooth mobility occurs and pain is not a feature. Following transplantation and reimplantation there is an early acute traumatic inflammatory reaction which may initiate root resorption and this may be followed by a non-specific chronic inflammatory reaction. Chronic inflammatory resorption of the root is associated with an adjacent area of radiolucency in bone. Long-term replacement resorption may also occur in which the progressive loss of root substance is matched by bony infilling. Root resorption is minimized in transplants with fully developed roots if they are root filled within 4 weeks of transplantation. Resorption of reimplanted teeth is generally more common and extensive than that seen in transplanted teeth and is largely a function of the length of time the tooth has been out of the jaw.
For teeth with immature roots, further development is dependent on revascularization of the pulp. The diameter of the apical foramen is a critical factor; teeth with a foramen greater than 1 mm diameter are more likely to revascularize.
Transplantation of a tooth from one site to another in the same individual (autotransplantation), into an extraction site or a surgically prepared socket, has been carried out for many years with varying degrees of success. Reimplantation is when a tooth is returned to its own socket, usually following traumatic avulsion. Transplantation of teeth from one individual to another of the same species (allografting) has been studied experimentally in animals but the results are very inconsistent because of graft rejection.
Autotransplants do not stimulate an immune response. Experimental studies in animals have shown that following transplantation or reimplantation the pulp and soft tissues attached to the root degenerate due to traumatic severence of the blood supply. In developing teeth with open apices, revascularization and repair of the dental papilla may occur and dentinogenesis may resume, although the dentine formed may be abnormal. However, continued root growth is rare. The reparative cells are probably derived from residual donor tissue which survives operative trauma. Reattachment of autotransplants may result from regeneration of the periodontal ligament, the formation of scar-like fibrous tissue running parallel to the root surface, or ankylosis. If ankylosis occurs the alveolar bone may be directly attached to the normal root surface or to resorption concavities. It has been suggested that preservation of the vitality of the periodontal ligament is an important factor in deterring root resorption and ankylosis.
Clinical studies of autotransplants in humans have concentrated mainly on root resorption which is the most commonly encountered complication. Sometimes the resorption is rapid, but more often is slowly progressive and periods of 10-15 years may elapse before resorption causes exfoliation of the transplanted tooth. Root resorption may be extensive before marked tooth mobility occurs and pain is not a feature. Following transplantation and reimplantation there is an early acute traumatic inflammatory reaction which may initiate root resorption and this may be followed by a non-specific chronic inflammatory reaction. Chronic inflammatory resorption of the root is associated with an adjacent area of radiolucency in bone. Long-term replacement resorption may also occur in which the progressive loss of root substance is matched by bony infilling. Root resorption is minimized in transplants with fully developed roots if they are root filled within 4 weeks of transplantation. Resorption of reimplanted teeth is generally more common and extensive than that seen in transplanted teeth and is largely a function of the length of time the tooth has been out of the jaw.
For teeth with immature roots, further development is dependent on revascularization of the pulp. The diameter of the apical foramen is a critical factor; teeth with a foramen greater than 1 mm diameter are more likely to revascularize.
Root fracture

The outcome of an intra-alveolar fracture of a root depends on several factors, which include the presence or absence of infection, the vitality of the pulp, the position of the fragments, the degree of comminution, the location of the fracture, and the mobility of the coronal fragment. If the fracture is sterile, three main patterns of healing may occur similar to those seen in the healing of a fracture of bone:
1. The root fragments become united totally, or in part, by calcified repair tissue resembling bone and/or cementum.
2. The fractured surfaces of each fragment become rounded off and clothed by cementum but are not united by calcified tissue. Fibrous tissue continuous with the periodontal ligament fills the intervening space (analogous to fibrous healing of a bone fracture).
3. The fracture surfaces become rounded and clothed by cementum as above but the fragments are widely separated. Fibrous tissue continuous with the periodontal ligament covers the fractured ends of the separate fragments and the intervening space is filled by alveolar bone (analogous to non-union of a bone fracture).
Key points - Autotransplantation and reimplantation of teeth
· success rates for autotransplantation higher than for reimplantation
· 85-95 per cent of autotransplants survive 5 years
· main complications are:
- root resorption - inflammatory/replacement types
- loss of pulp vitality in teeth with immature roots
- failure to complete root development in teeth with open apices
- poor periodontal healing
The pulp chamber in either fragment may become obliterated by calcified tissue.

The outcome of an intra-alveolar fracture of a root depends on several factors, which include the presence or absence of infection, the vitality of the pulp, the position of the fragments, the degree of comminution, the location of the fracture, and the mobility of the coronal fragment. If the fracture is sterile, three main patterns of healing may occur similar to those seen in the healing of a fracture of bone:
1. The root fragments become united totally, or in part, by calcified repair tissue resembling bone and/or cementum.
2. The fractured surfaces of each fragment become rounded off and clothed by cementum but are not united by calcified tissue. Fibrous tissue continuous with the periodontal ligament fills the intervening space (analogous to fibrous healing of a bone fracture).
3. The fracture surfaces become rounded and clothed by cementum as above but the fragments are widely separated. Fibrous tissue continuous with the periodontal ligament covers the fractured ends of the separate fragments and the intervening space is filled by alveolar bone (analogous to non-union of a bone fracture).
Key points - Autotransplantation and reimplantation of teeth
· success rates for autotransplantation higher than for reimplantation
· 85-95 per cent of autotransplants survive 5 years
· main complications are:
- root resorption - inflammatory/replacement types
- loss of pulp vitality in teeth with immature roots
- failure to complete root development in teeth with open apices
- poor periodontal healing
The pulp chamber in either fragment may become obliterated by calcified tissue.
Age changes in teeth
Introduction
Age changes in teeth include changes in morphology associated with wear, especially attrition, and changes in structure and composition of the dental hard tissues. Age changes in the dental pulp are discussed in.
Enamel
The enamel tends to become more brittle and less permeable with age, reflecting the ionic exchange which occurs between enamel and the oral environment throughout life. Darkening of the enamel has also been described and may be due to absorption of organic material.
Dentine
The two main age-related changes in dentine are continued formation of secondary dentine resulting in reduction in size and in some cases obliteration of the pulp chamber, and dentinal sclerosis associated with the continued production of peritubular dentine. Both of these processes are also associated with caries and tooth wear. Sclerosis of radicular dentine tends to make the roots brittle and they may fracture during extraction. It is also associated with increasing translucency of the root. This starts at the apex in the peripheral dentine just beneath the cementum and extends inwards and coronally with increasing age. The length of root affected by translucency is used in forensic dentistry as one method of age estimation.
CementumIntroduction
Age changes in teeth include changes in morphology associated with wear, especially attrition, and changes in structure and composition of the dental hard tissues. Age changes in the dental pulp are discussed in.
Enamel
The enamel tends to become more brittle and less permeable with age, reflecting the ionic exchange which occurs between enamel and the oral environment throughout life. Darkening of the enamel has also been described and may be due to absorption of organic material.
Dentine
The two main age-related changes in dentine are continued formation of secondary dentine resulting in reduction in size and in some cases obliteration of the pulp chamber, and dentinal sclerosis associated with the continued production of peritubular dentine. Both of these processes are also associated with caries and tooth wear. Sclerosis of radicular dentine tends to make the roots brittle and they may fracture during extraction. It is also associated with increasing translucency of the root. This starts at the apex in the peripheral dentine just beneath the cementum and extends inwards and coronally with increasing age. The length of root affected by translucency is used in forensic dentistry as one method of age estimation.
Cementum continues to be formed throughout life, especially in the apical half of the root, resulting in a gradual increase in thickness to compensate for interproximal and occlusal attrition. The amount of secondary cementum at the apex of a tooth is another factor that can be taken into account in forensic dentistry in age estimation, but it is important to distinguish between physiological apposition with age and other causes of hypercementosis.
Key Words : teeth whitening teeth cleaning wisdom teeth removal wisdom teeth extraction gold teeth false teeth bad teeth teeth bleaching
Tidak ada komentar:
Posting Komentar